This past Wednesday marked one month since my surgery, which is a little hard to believe. After we got the great-news pathology results a few weeks back, I decided to take a short break from writing. Once we had those results and could take something of a deep breath, it felt good to distance myself as much as possible from anything cancer-related. The blog has been a wonderful way to connect with people, but a brief sabbatical felt nice.
A lot has happened in the way of recovery! I got my staples out — a small thing, maybe, but a big relief in how it accelerated the healing of my incision. A few nights ago, I cheered heartily after injecting myself with the last of a month’s worth of nightly Lovenox shots (for prevention of blood clots). I’m basically pain-free now, other than the occasional cramping at night (still haven’t fully figured that one out, but eating a much earlier dinner seems to have helped) and (who would’ve thought?) whenever I sneeze. I still get tired pretty easily, but I can walk around the neighborhood at a respectable clip, pretty much to my heart’s content.
The ileostomy bag and I are still joined at the hip (sorry), getting along much better now. I had a bit of an issue they call a “separation,” where the skin around the stoma doesn’t heal after the stoma retracts to its smaller post-surgery size. (For a while after surgery, the stoma is very swollen from all the action — in my case, probably twice the size it has settled down to now.) With a little powder and some invaluable guidance from Rose, my amazing ostomy nurse, it’s nearly fully healed now.
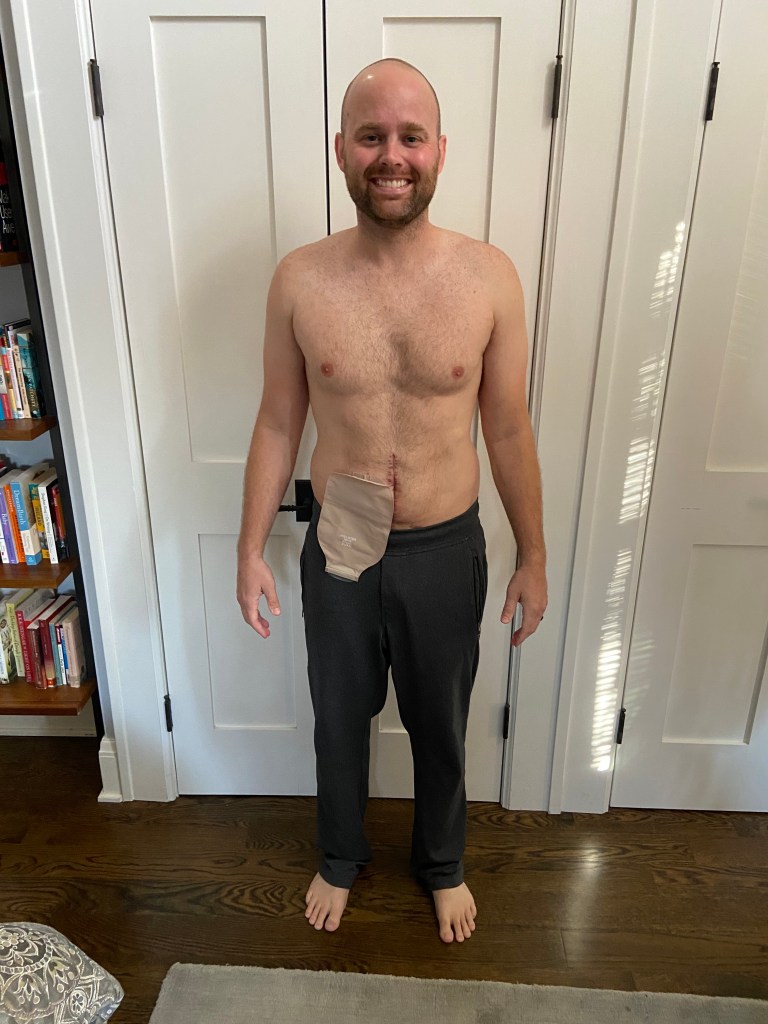
My required low-fiber, “soft” diet has definitely been the weirdest part about this period of recovery. If you were following the blog in the days not long after my diagnosis, I decided very quickly to fundamentally change my diet: no more red meat or fried food, generally very veggie-forward, etc. The irony is that until my next surgery, I basically can’t eat fruits or veggies (in addition to nuts, seeds, and anything else that doesn’t easily break down during digestion) — the risk of things getting blocked is too great.
So, while it was tough to accept, I’ve basically had to pause the new and improved diet. It’s been lots of chicken, pasta, and rice these last few weeks. Because my options are so limited right now, I’ve even allowed myself the occasional burger, or ice cream bar. I get hungry constantly, but I can’t eat nearly the quantity I could before (as Alexis has correctly pointed out, this is arguably the biggest blessing of my new condition), which means I have to eat pretty frequently.
I’ve still stayed away from alcohol, but when it comes to caffeine, the fatigue from weeks of crappy sleep has forced me to venture a bit beyond green tea into an occasional latte or mocha. I’m trying hard not to slip back into my old habits, but a little bit of careful comfort eating has felt well worth it during this stretch. On the plus side, I left the hospital at 185 pounds (down from 205 pre-diagnosis) and have stayed there since. Hey, it’s not a weight loss plan I’d ever recommend, but it sure worked!
Tomorrow I’m heading back to work. I’m planning to take things slow, and I know I’m going to have to be very mindful of not pushing myself back to my pre-diagnosis pace. I’m going to be diligent about taking breaks, eating regularly, prioritizing sleep, and not getting worked up over problems that aren’t really problems — all the things I used to do very poorly. Frankly, I’m nervous about how that’s all going to go. But I miss my colleagues, many of whom are dear friends, and I’m craving some intellectual stimulation and the beginnings of a return to normalcy.
It’s only been two-and-a-half months, but I feel like a kid staring at the ceiling the night before the first day of eighth grade. Time to go finish my summer reading.
